
Simulated practice is an opportunity to transition nursing students from on-campus learning to clinical practice. There is limited evidence on simulated practice’s role in assisting this transition at the beginning of a nursing student’s education in terms of benefits, challenges, differences and affordances. This study aimed to research the impact of a simulated practice programme as a transitioning tool for first-year paediatric nursing students.
A participatory action research approach was used to address challenges in student’s transitioning to clinical practice and a lack of clinical placement capacity. A low-technological (physical), high-authenticity (emotional and environmental)-simulated practice programme for first-year paediatric nursing students was implemented. Forty students across two cohorts were recruited, and a qualitative survey was completed post-simulation/pre-clinical practice and post-clinical practice. Reflexive thematic analysis was used to develop the resulting themes.
There was an initial 93% response rate after the simulated practice and 88% after clinical placement. Eight themes (‘bridging’ from simulation to practice and to enhance practice; ‘preparedness’ once on clinical placement; ‘applied learning’ reliably transferred to practice; ‘skill decay’ between simulation and practice; ‘same but different experiences’ between simulation and practice; simulation and clinical ‘practice pace’; ‘safety’ of simulation; and ‘unique affordances’ of simulated practice) were constructed from the data, and an additional nine sub-themes were identified (transference to practice; practice enhancement; slow-motion care; hectic; it is safe; it was safe; feedback and reassurance; practice and practice; and unpressured). Collectively, the themes indicated that simulated practice in this context is conveyed as a well-being tool in addition to having experiential learning and bridging benefits.
This study revealed that simulated practice can assist in transitioning paediatric student nurses to clinical practice. It identified its value in terms of fostering holistic learning, well-being and bridging theory to practice. To ensure long-term effectiveness, simulation maintenance training, booster training and refresher strategies should be included as part of the programme to prevent skill decay. Future studies should consider isolating these key findings for a more in-depth look at their meaning.
Clinical skills are an essential part of healthcare provision and nursing education. Traditionally, nurse educators have relied on clinical placements to provide practical and contextual experiential learning opportunities [1]. There are, however, a range of practical restrictions that come with clinical placement; for example, only a limited number of students can be on clinical placement at any one time. At a time when healthcare workforce shortages are reported, the need to train more nurses is vital. However, the constrained capacity of clinical placements has been long recognized as an issue in many countries trying to meet this increasing demand [2]. The need to identify alternative ways to train nurses and healthcare practitioners that enhances, not replaces, clinical practice is even more pressing given the increased pressure and safety concerns that the COVID-19 pandemic has created in healthcare settings [3,4].
Simulation is now widely used in nursing education [5]. Like clinical placements, simulation is a form of experiential learning [6]. Students can learn and practice clinical skills in a simulated environment, with a range of equipment and simulated patients that approximate a clinical setting [7]. Simulation, as a pedagogical strategy, has several advantages over traditional didactic approaches, one being that it allows students to apply the cognitive and psychomotor skills required to competently undertake clinical tasks [8]. Furthermore, simulation allows students to practice these skills in a safe, supportive environment before entering clinical placement. This allows students to safely make mistakes, which will not impact care, and to receive constructive feedback, further enhancing critical reflection and self-awareness, which are important skills in themselves.
In 2014, a study in the USA concluded that up to 50% of clinical placement could be effectively substituted by simulation in core nursing courses [9]. Further studies have shown that there is no significant difference in student outcomes in relation to clinical competency, knowledge and confidence when using simulation to replace a percentage of clinical practice [10–13]. Student perceptions of simulation compared with clinical placement have also been explored and have been deemed positive overall [14–16]. Several studies have examined the role of simulated practice in assisting student nurse’s transition to clinical practice as new graduates rather than as students at the beginning of their educational journey [17–21].
While simulation has a number of benefits and the potential to address workforce and training-related issues, a large amount of the literature has focused on simulation when used to train for specific high-risk, rare events (e.g. resuscitation) and in high-technological settings. Broadly, high-technological simulation utilizes sophisticated technology and mannequins to recreate a clinical scenario as closely as possible [21,22]. The drawback of such an approach is that it can be expensive, resource-intensive and may not always meet the required learning needs [23,24]. This contrasts with low-technological simulation, which uses simple, low-cost alternatives and often sources everyday materials to simulate a clinical environment [25]. In this study, the terms high- and low-technological simulation are used rather than high and low fidelity, as fidelity is a multi-dimensional concept that incorporates the physical (technology), environmental and emotional aspects of the simulation design and, therefore, should not be a judgement on realism unless incorporating all three dimensions at a minimum [26].
The focus of training for first-year UK nursing students is the development of fundamental nursing skills aimed at facilitating their transition to clinical practice. Low-technological-simulated practice offers simple, safe, low-cost settings to recreate common, realistic and relevant clinical scenarios within the scope of the knowledge and skills required for this cohort. Beyond this, there is an increasingly pressing need to explore the potential of simulated practice as a pre-registration training tool, given that the nursing workforce expansion is a priority [27], and there are already limited clinical placements. Placement experience may not always meet the learning needs of students but instead meet a registration requirement focussed on hours rather than opportunities [4]. By engaging students who have had no clinical practice experience, there is an opportunity to identify if simulation is a reliable tool to enhance the transition into clinical practice.
The aim of this study was to research the impact of a low-technological, high-authenticity-simulated practice programme on a UK first-year children’s nursing pre-registration programme. In this study, the authors sought to determine the programmes use as a transitioning tool to clinical practice and to identify the benefits, challenges, differences and affordances.
What are the key challenges, differences and affordance of implementing simulation prior to first clinical placement in a pre-registration children’s nursing programme?
This study utilized a participatory action research approach [28], whereby practitioners (in this case academic faculty) identified a problem and used their own knowledge to conceptualize it (student challenges in transitioning to clinical practice, lack of suitable clinical placement capacity) and provide a solution (a customized simulated practice environment) (Table 1). The solution was then implemented and evaluated qualitatively. The reporting of this study follows COREQ guidance [29].

| Simulation element | Descriptor | ||
|---|---|---|---|
| Participant orientation | UK first-year student nurses studying for their BSc (Hons) Nursing (child) were expected to wear uniform when attending simulated practice and to behave professionally at all times. They were expected to plan the care they would be expected to provide as first-year nursing students on clinical placement. Students were assigned patients and a nursing care task; they were told to work in pairs and were encouraged to challenge each other as to their approach. For example, why use an oral thermometer on a toddler. | ||
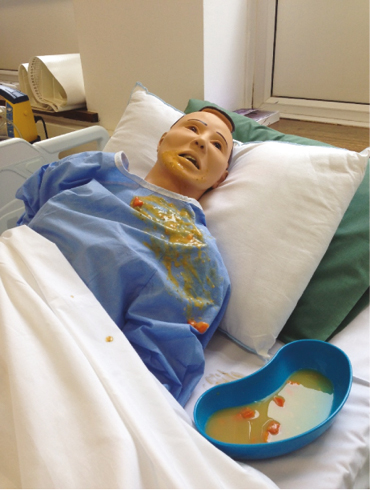
| Simulator type | Low-technological mannequins of varied ages were utilized. Creative solutions were employed to simulate different clinical conditions by using low-cost household resources. For example, mustard seeds, mint-gel and mustard paste simulated the appearance and consistency of neonatal diarrhoea in a nappy, canned vegetable soup simulated vomit and tea simulated urine. | ||
 |
 |
 |
|
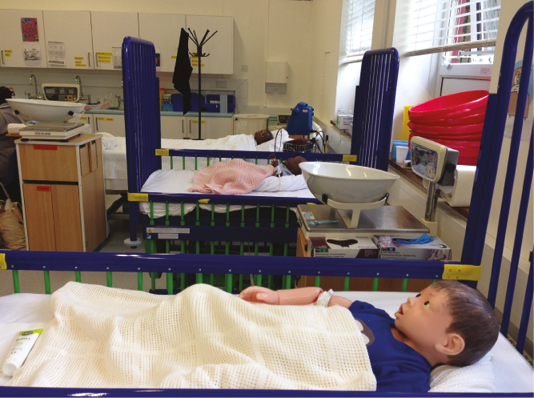
| Simulation environment | The simulation was university based within the skills labs, which were adapted to represent children’s wards. Rooms were modified and thoughtfully equipped to mirror a ward environment. | ||
 |
 |
 |
|
| Simulation scenario | The scenarios evolved slowly over a six-day period allowing the students to develop and rehearse the knowledge and skills they acquired. There were a total of eight patients on the ward each day. Ranging in ages from 20 days to 15 years. The patients had non-complex conditions such as whooping cough, pneumonia, epilepsy, fractured femur, acute asthma attack, minor burns, appendectomy and salmonella. Day 1: Handover, carry out vital observations (plus neurological observations where required) and documentation, admit new patients (some with D&V and therefore PPE required), complete admission assessment and care plan development. Debrief at end of the day. Day 2: Same as day 1 plus implement care plans created the previous day and care for new patients being admitted. Debrief at end of the day. Day 3: Same as days 1 and 2 plus medicine management (administer medicine to all patients, checking the prescription chart, calculating the dosage and using an appropriate clinical hold). Debrief at end of the day. Day 4: Continuing with shift tasks and patients admitted previously plus wound dressing using non-touch technique (scald on the chest, a laceration to the head). Debrief at end of the day. Day 5: Continuing with the same patients as day 4 plus new admissions. Focus on communication through managing phone calls (calls received from health professionals, family members and clinical reports). Plus prep a patient for theatre. Debrief at end of the day. Day 6: Same patients and tasks as day 5 plus a focus on managing confrontation. The scenario led to talking to parents. For example, explain home safety to the mother of the child with the scald, explaining why the teenager in isolation couldn’t come out of the room, deescalating the father who did not have access to his son without a social worker and who just burst onto the ward. Debrief at end of the day. Final debrief for the entire period. Throughout the period, students would care for different patients which enabled them to rehearse and practice the various skills and knowledge they have obtained. At the end of the last shift, they were able to choose which patient they wanted to care for to fill any gaps in knowledge or skills. |
||
| Instructional design | The scenarios were mapped around the UK’s Nursing and Midwifery councils (NMC [31]) five essential skills clusters to ensure students developed and rehearsed a range of skills required for safe and effective practice. Dedicated clinical scenarios, feedback and debrief-type discussion were included to reinforce core nursing and children’s-nursing-specific skills. Aspects of the patient care were broken down and delivered at a slower pace than they would be in reality. This created an environment for peer support, learning and discussion in a safe environment. The students had time to plan their care and discuss with both their peers and the facilitators the rationale for their actions. To address the complex construct of employability, the focus was also extended to ‘soft transferable skills’ such as efficient communication with patients, establishing a therapeutic relationship with parents/relatives, gaining trust and showing compassion. These were supported by customized role-play interventions that help students appreciate the different perspectives (patient, parent/carer, healthcare professional) and enabled them to practise key attributes of a successful children’s nurse, including managing themselves (in a stressful environment), others (colleagues, the agitated parent), information (communicating accurately while ensuring confidentiality) and the task (prioritization). Students undertook two consecutive weeks of simulated practice totalling 45 hours spread over 3 days per week (7.5 hours per day) in their first semester. In addition, they had a workbook to complete as independent study which was a reflection of the simulation activities. The scenarios were developed on a daily basis; initially, the focus was on one core skill per scenario. However, this was gradually built up to combine several core skills for total patient care. Each day building on and reinforcing the previous day’s simulation. This allowed the students to rehearse and perfect the core skills. |
||
| Feedback/debriefing | Feedback was a constant feature of the simulation. For example, every day started with a handover, followed by a discussion to establish understanding of the handover. The students could ask the facilitator at any point for guidance, which they did. This resulted in small feedback sessions between the facilitator and two students. At the end of each day, there was a verbal debrief with the whole group asking the students what they had learnt, and what they felt had gone well. Facilitators consisted of three experienced academics in the field of nursing education, who had an established teacher–student relationship with the study participants. There was a five-to-one student-to-staff ratio. |
||
Two cohorts (intakes per year) of first-year student nurses enrolled in a Bachelor of Science (Honours) Nursing (Child) programme were recruited (20 per cohort, 40 in total). There was no difference amongst cohorts in terms of experience. We included both cohorts to ensure a breadth of data and perspectives in line with previous studies [32]. Purposive sampling was used to intentionally select participants (first-year cohorts, pre-clinical practice) who were required to undertake the simulation activity under study and, therefore, answer the study research question. There were no differences in terms of clinical experience across the cohorts, and students had no prior experience of simulation.
Students undertook two consecutive weeks of simulated practice totalling 45 hours spread over 3 days per week (7.5 hours per day) in their first semester. In addition, they were required to complete a workbook as independent study which was a reflection of the simulation activities. During the simulations, low-technological mannequins of varied ages were utilized. Creative solutions were employed to simulate different clinical conditions by using low-cost household resources (Table 1).
Students completed an open-ended survey at two points in time, after the initial simulation in the first semester (pre-clinical placement), and after they completed their first clinical placement (post) 10 weeks later. The survey was developed based on:
In the first survey, students were asked to complete a series of questions designed to elicit qualitative data related to their experiences of simulation: what they had learnt, their confidence and the perceived advantages and challenges of simulation. After completing the clinical placement, students completed another survey where they were asked about the skills they had applied whilst on placement, how placement compared with simulation and again the perceived advantages and drawbacks of simulation.
A reflexive thematic analysis was conducted drawing on the team’s different experiences in nursing and simulation to generate shared meaning [34]. MAXQDA2020 software was used to assist in analyzing the pre and post data [35], by identifying patterns amongst the data and generating coding maps where semantic networks were formed that revealed thematic relations pertaining to the research questions through interconnected codes. All authors had input to the process.
This research was approved by the University of Greenwich Human Research Ethics Committee (reference number: UREC/15.5.5.10).
Thirty-seven pre-placement students and 35 post-placement students completed the surveys, respectively (93% response rate and 88% after follow-up). Eight core themes (‘bridging’ from simulation to practice and to enhance practice; ‘preparedness’ once on clinical placement; ‘applied learning’ reliably transferred to practice; ‘skill decay’ between simulation and practice; ‘same but different experiences’ between simulation and practice; simulation and clinical ‘practice pace’; ‘safety’ of simulation; and ‘unique affordances’ of simulated practice) that reflected both the pre- and post-clinical placement perspectives were constructed from the data, and an additional nine sub-themes were identified (transference to practice [pre]; practice enhancement [post]; slow-motion care [pre]; hectic [post]; it is safe [pre]; it was safe[post]; feedback and reassurance; practice and practice; and unpressured). Figure 1 provides a thematic model of the themes that were constructed and categorized according to the research aims. A description of the themes is reported below.


Transitioning: simulation practice to clinical practice.
The coding of the data identified a ‘bridging’ theme that had two components. Firstly, ‘transference to practice’ (sub-theme) where students were linking specific aspects of their simulated practice experience directly to their future placements, revealing a degree of potential for the simulated practice to have a direct bridging effect. The direct transfer potential of the learning in simulated practice to future placements included areas related to relationship building, initiative taking, confidence, technical skills acquisition, language and a general enthusiasm for both simulation and clinical practice:
I will strike up conversations when I go into practice and chat with patients and families to help build a therapeutic relationship. I am less hesitant to do so now
Secondly, a ‘practice enhancement’ (sub-theme) revealed how simulated practice was an opportunity for students to enhance what they had already learnt in practice, or try things they had not had the opportunity to try in practice:
It was beneficial to me because I had come across some of the things in practice before but didn’t know what to do e.g. what information you can and can’t share with who
This theme revealed that once on placement, students felt that the simulated practice had prepared them, this was described in many ways, from specific skills to confidence and an overall understanding of clinical practice, as well as reducing anxiety.
This made me a lot more relaxed when I started in the wards and prevented a lot of anxiety
Many students gave specific examples of what they had learned during simulated practice that they applied to their clinical placements. This provided reliable evidence that the learning had been transferred:
Yes. I have applied my skills to the drug calculations, answering telephone queries, bed-making, correct way to clean, observations
Another theme identified was in relation to potential ‘skill decay’ between simulation and clinical practice. Participants also revealed how this could be mitigated in the future:
Depending on where you are on placement some of the techniques you learn cannot be practiced and there is a tendency to forget because of lack of use
Every person will have different placements so for some people some topics covered in simulation will come ‘late’ and for some ‘too early’
A theme of ‘same but different’ emerged from the data related to the simulation design. This highlighted key areas where the simulated practice mirrored practice and where it was different more generally. Similarities related to equipment, scenarios and the skills that were targeted. Differences were in relation to being able to control the simulated environment, therefore exposing the students to more than what they would have potentially been exposed to in practice:
Very close to reality as in simulations we used similar equipment that we used out in placement
The environment isn’t controlled in practice, therefore there is more pressure. It is also awkward doing some obs
Another theme that was developed in relation to the key differences between simulated practice and clinical practice was: ‘Practice pace’, where simulated practice was seen as ‘slow-motion care’ and clinical practice was viewed as ‘Hectic’ (sub-themes).
The benefits were excellent of SP [simulated practice]. It was slow-motion care so I was able to think more and follow actions through correctly
The benefits of this were that I was able to feel safe enough to voice any concerns I felt I was able to go through things for as many times as I needed, whereas in practice, I didn’t have much time to go over things
In practice everything is faster and more hectic but it was helpful to have had the opportunity to do things at a slower speed and we had the time to ask questions in detail
Everything is much faster in clinical practice. I felt more pressure to do tasks well in practice but in the simulations I felt at ease
Another theme that highlighted key differences between simulated practice and clinical practice was in relation to ‘Safety’, ‘it is safe’ (stated during simulated practice), and ‘it was safe’ (stated from a reflective clinical practice perspective on simulated practice) [sub-themes]. This highlighted the general feeling of safety that simulated practice enabled both during simulated practice and on reflection.
Yes, I felt I was able to make mistakes during simulation and was taught the correct way without judgement or annoyance
My confidence has definitely improved because SP [simulated practice] was a safe environment and the mistakes I made here I have learned from as well as from others mistakes and really good strategies of others
It was a safe place for me to get things wrong
It felt easier to learn how to do things [in simulation] and more relaxed as it wouldn’t matter if there were any mistakes made
In addition, the analysis revealed three unique affordances of simulated practice: ‘feedback and reassurance’, ‘practice and practice’ and ‘unpressured’.
Having feedback from teachers and fellow students was constructive and impersonal – I think that this was a much kinder introduction to answering the phone in front of them rather than at the nursing station
It gave us a chance to practice and practice until we understood how the equipment worked
The benefits of simulated practice I felt were much greater as opposed to practice at each situation, methods and clinical skill was explained fully and I did not feel pressured as I would in practice to get things right the first time
The two themes of bridging and preparedness that emerged in this study spoke to the transitioning benefits of student’s simulated practice experiences to their clinical practice. Previous studies have aimed to identify if simulation bridges the theory–practice gap for graduate nurses; however, these studies have focused on its ability to ‘scaffold’ the learning experience in preparation for practice [36,37] and relied on students’ perceptions of simulation as a transitioning tool more generally [38–40]. This study is the first to provide evidence of first-year nursing students consciously linking their simulation experience to their clinical practice. The pre-simulation and post-clinical practice nature of this study has provided evidence of simulation’s ability to aid student’s transition to clinical practice which has transferability potential to other contexts. More specifically, it has highlighted the value of a low-technological, high-authenticity simulation design’s value for this purpose.
Students expressed that simulated practice was an anxiety-reducing tool when it came to clinical practice. This is in direct contrast to much of the medical literature in this area that presents simulation as ‘anxiety provoking’ [24,41–43]. This study included many of the recommendations for mitigating anxiety in simulation evident in the literature such as creating a safe learning environment, developing trusting relationships and supporting performance expectations [44–46]. This is further evident in the ‘applied learning’ theme where students had directly transferred their learning from the simulated practice to clinical practice by using concrete examples. This helps answer the research question as to whether this specific programme was beneficial in transitioning first-year pre-registration paediatric nurses to clinical practice. This study revealed that the programme provided the students with additional learning opportunities compared with clinical practice in terms of more exposure and opportunity to undertake skills and practice communication techniques. The use of a simulated practice programme can, therefore, not only prepare students for practice, but also enhance their experience once in practice, as well as provide them additional opportunities that they may not get on clinical placement.
Conversely, the study highlighted the challenges associated with the potential for skill decay if the clinical practice following the simulated practice did not provide an opportunity to practice what they had learnt, or if the time between both experiences was too long. This is a legitimate concern for educators when utilizing simulation programmes in this context. Sullivan et al. [47] provided a framework that aimed to mitigate these issues through the use of simulation maintenance, booster and refresher training strategies. It is suggested that similar programmes include these strategies as part of simulation design considerations. This revelation has provided a valuable addition to the current programme.
The ‘practice pace’ theme highlighted the students differing experience between simulated and clinical practice with the language of ‘slow-motion care’ and ‘hectic’ giving a sense of learning preference towards the simulated practice experience over the clinical practice experience. Ironically, simulation is often designed to mimic the pace of clinical practice; however, these data have revealed that students valued the opportunity to undertake a slowed-down version of clinical practice. This questions elements of simulation design in relation to ‘fidelity’ and the choices made in what is replicated and what is deliberately changed to create better learning opportunities. This outcome aligns with Escher et al. [48] who in their study on methods related to simulation-based teamwork training concluded that novices may gain from a slower tempo simulation experience.
A feeling of safety in both pre- and post-clinical placement in relation to simulated practice was reported in this study. Psychological safety and safe environments are often emphasized amongst the simulation literature [49,50]; however, less emphasis is put on the feelings of safety it provokes for students in relation to clinical practice. This highlights another unique affordance of simulated practice in enabling constructive feedback and reassurance, opportunities to ‘practice and practice’ and an unpressured environment. This provides a clear rationale as to why simulated practice is beneficial in its own right and not just a means to replace clinical practice.
Collectively, the themes of safety, anxiety-reduction, slow-motion care, preparedness, constructive feedback and reassurance, and reduced pressure reveal that simulated practice in this context can be seen as a well-being tool in addition to having experiential learning and bridging benefits.
This was a small study that included two groups of students at one point in time in their training from one higher education institute, and, therefore, the outcomes are specific to the context presented. However, there is the potential for the results to be transferable to other institutions with learners at a similar stage in their training and with a similar course structure.
This qualitative study has provided evidence that simulated practice can help transition first-year paediatric student nurses to clinical practice. It has revealed the benefits of simulated practice as an educational tool, its similarities and differences to clinical practice and its potential challenges, as well as unique affordances. The low-technological, high-authenticity design of the simulation programme examined in this study was clearly appropriate for the learner’s requirements and enabled students to link between their simulated practice and clinical practice experiences.
The research team consisted of six experienced academics in the field of simulation, nursing and healthcare research and education, with a range of 5 to 20 years of experience. Two of these academics (NN and HS) conceptualized and realized the simulated practice intervention and had an established teacher–student relationship with the study participants and another two academics/researchers, without direct teaching commitments for this student cohort (CM and KC) theorized and realized the research design, to ensure no bias or conflict of interest. SMW and RE conducted the study analysis, and write-up of the results with input from all authors.
This research was supported by the University of Greenwich.
The datasets used and/or analyzed during the current study are available from the corresponding author on reasonable request.
This research was approved by the University of Greenwich Human Research Ethics Committee (reference number: UREC/15.5.5.10).
Not applicable.
The authors declare that they have no competing interests.
The team comprised female academics, as representative to the nursing profession, with a range of research experience, and from a predominantly white middle-class background, with one Black academic and one male academic. All researchers strongly advocate simulation in healthcare teaching which could have introduced unconscious bias in data collection and analysis. However, they worked independently and collaborated towards the end of the study to minimize bias. The researchers who worked on conceptualizing and implementing the simulation programme were senior educators in nursing and had a strong relationship with the student participants, through an educator–student bond. The researchers responsible for conceptualization and implementation of the study had a unique insight into the student needs and clinical placement capacity, creating a customized programme aligning to national guidelines on simulation in lieu of clinical practice. The researchers involved in recruitment and data collection did not have a prior relationship with the students. There was no coercion to participate in the study. The main researcher for data collection was a senior academic from another healthcare discipline (radiography), with a strong interest and expertise in simulation, which allowed them to see the work through a different interpretative lens and gain the students’ trust as an experienced researcher, independent to the students’ learning journey. The researchers working on data analysis worked separately from those who worked on design, implementation and data collection but they regularly met online to discuss findings.
1.
2.
3.
4.
5.
6.
7.
8.
9.
10.
11.
12.
13.
14.
15.
16.
17.
18.
19.
20.
21.
22.
23.
24.
25.
26.
27.
28.
29.
30.
31.
32.
33.
34.
35.
36.
37.
38.
39.
40.
41.
42.
43.
44.
45.
46.
47.
48.
49.
50.